For the patient with and/or at risk for pressure ulcers, in addition to assessing M2250 Pressure Ulcer care and prevention on OASIS C home health care forms, also include these MyHomecareBiz Best Practice assessment strategies:
Best Practice Assessment Strategies for Pressure Ulcer Risk1. Determine the client’s general condition of the skin.
2. Assess the client’s nutritional status, including weight, weight loss, and serum albumin levels, if indicated.
3. Assess the client’s awareness of the sensation of pressure.
4. Assess for fecal and urinary incontinence.
5. Assess patient’s mobility.
6. Assess for environmental moisture (excessive perspiration, high humidity, wound drainage).
7. Assess the amoun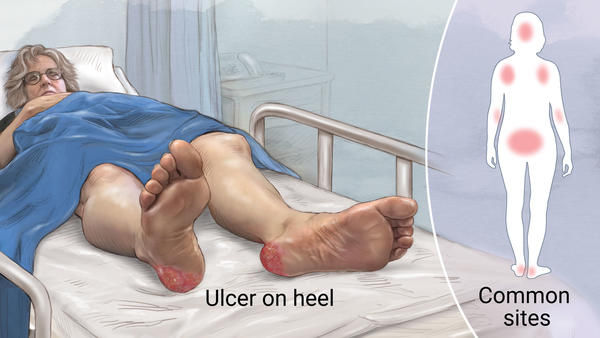
8. Assess the surface that the clients spend a majority of time on (mattress for bedridden clients, cushion for clients in wheelchairs).
9. Assess the skin over bony prominences (sacrum, trochanters, scapulae, elbows, heels, inner and outer malleolus, inner and outer knees, back of the head).
10. Perform pressure ulcer risk assessment: Braden scale, Norton scale.
11. Assess the client’s level of pain, especially related to dressing change and procedures.
12. Assess and stage the pressure ulcers.
(M2250) Plan of Care Synopsis: f. Intervention(s) to prevent pressure ulcers
If the physician-ordered Plan of Care includes planned clinical interventions to reduce pressure on bony prominences or other areas of skin at risk for breakdown, select “Yes.”
Planned interventions include teaching on frequent position changes, proper positioning to relieve pressure, careful skin assessment and hygiene, use of pressure-relieving devices such as enhanced mattresses, etc.
If the clinician completed a formal or informal assessment that indicated the patient is not at risk for pressure ulcers, select “NA” (unless orders for interventions to reduce pressure on areas of skin at risk for breakdown are present). If more than one pressure ulcer risk assessment was completed by the assessing clinician, all must be negative in order to select “NA.”
(M2250) Plan of Care Synopsis: g. Pressure ulcer treatment based on principles of moist wound healing OR order for treatment based on moist wound healing has been requested from physician
If the physician-ordered Plan of Care contains orders for pressure ulcer treatments based on principles of moist wound healing (for example, moisture retentive dressings) OR if such orders have been requested from the physician, select “Yes.”
If the patient has no pressure ulcers OR no pressure ulcers needing moist wound healing treatments per physician, select “NA” (unless orders for pressure ulcer treatments based on principles of moist wound healing are present).
Moist wound healing treatment is any primary dressing that hydrates or delivers moisture to a wound thus promoting an optimal wound environment and includes films, alginates, hydrocolloids, hydrogels, collagen, negative pressure wound therapy, unna boots, medicated creams/ointments.
For more information on Medicare's Home Health Care Quality Indicators click here.

